Data from the American Hospital Association shows that hospitals were not overwhelmed in 2020
Despite warnings that hospitals would be overrun due to COVID, hospital utilization decreased in the United States
In a previous post, I wrote about how seroprevalence studies have shown that COVID-19 was not much worse than the flu for the majority of the population. Yet, if you spoke with nurses or health care professionals, or followed the narratives promoted by the government and their media acolytes, you would have thought the disease was far worse.
Hospitals were overwhelmed, we were told. Nurses were overworked. And there was not enough room for the throngs of COVID patients flooding the hospitals.
Now, two years after the start of the pandemic, we have the data from 2020 that can help us determine just how overwhelmed the hospitals actually were.
Hospital Utilization
Since 2014, the American Hospital Association has collected data from all community hospitals in every state in the U.S. If the hospitals truly were overwhelmed, we should expect to see higher hospital utilization in 2020 than in previous years.
Rather than plot the data from every single state, I went ahead and chose 15 states that offer a good representation of what was going on in the country: Illinois, California, Colorado, Georgia, Florida, Idaho, Kansas, Louisiana, Massachusetts, Michigan, Nevada, New York, South Dakota, Texas, and Vermont.
If the mainstream narrative was correct, we would expect U.S. states that didn’t lock down or that opened back up early to have much higher hospital utilization than in previous years. South Dakota, the only state with no restrictions, should have had skyrocketing hospital utilization. Florida, Georgia, and Idaho opened early and should have also had higher levels. Lockdown states such Michigan, New York, Massachusetts, and California should have utilization about on par with previous years.
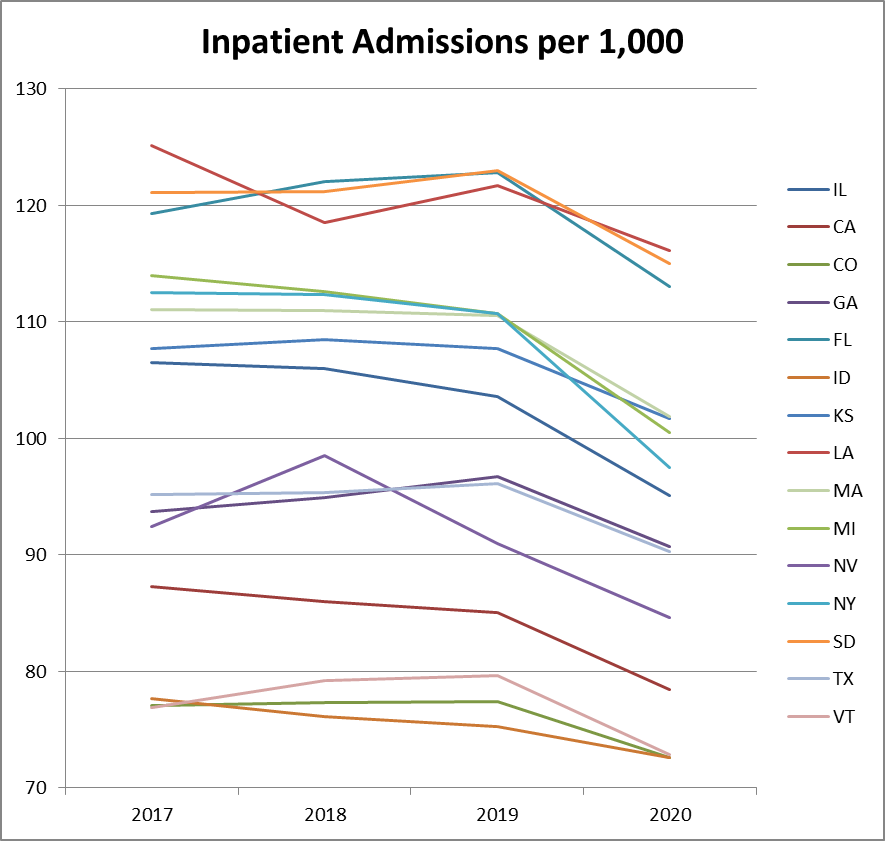
Below are the number of inpatient admissions and outpatient visits per 1,000 population in the selected states. All numbers are normalized to the respective state populations from the 2020 Census.
As you can see, most states had a significant decrease in inpatient admissions and outpatient visits in 2020. There doesn’t seem to be any sort of correlation between the number of government imposed restrictions and hospital utilization. The free state of South Dakota had a decrease in overall hospital utilization, just like nearly every other state in the Union. It seemed that COVID did not bring the catastrophe to South Dakota hospitals that the media was constantly warning about. The same went for freer states such as Florida, Texas, Georgia, and Idaho.
The reason for the decrease in hospitalizations is obvious. Hospitals, whether voluntarily or under state coercion, delayed elective surgeries and routine screenings to make way for the flood of COVID patients. Based on the numbers, however, the flood never came.
It is not uncommon during a bad flu season for hospitals to cancel elective surgeries for a few days. The difference in 2020 was that these cancellations lasted for months. Based on typical utilization levels, it looks like implementing this policy for such a long period of time was unnecessary.
Capacity and Personnel
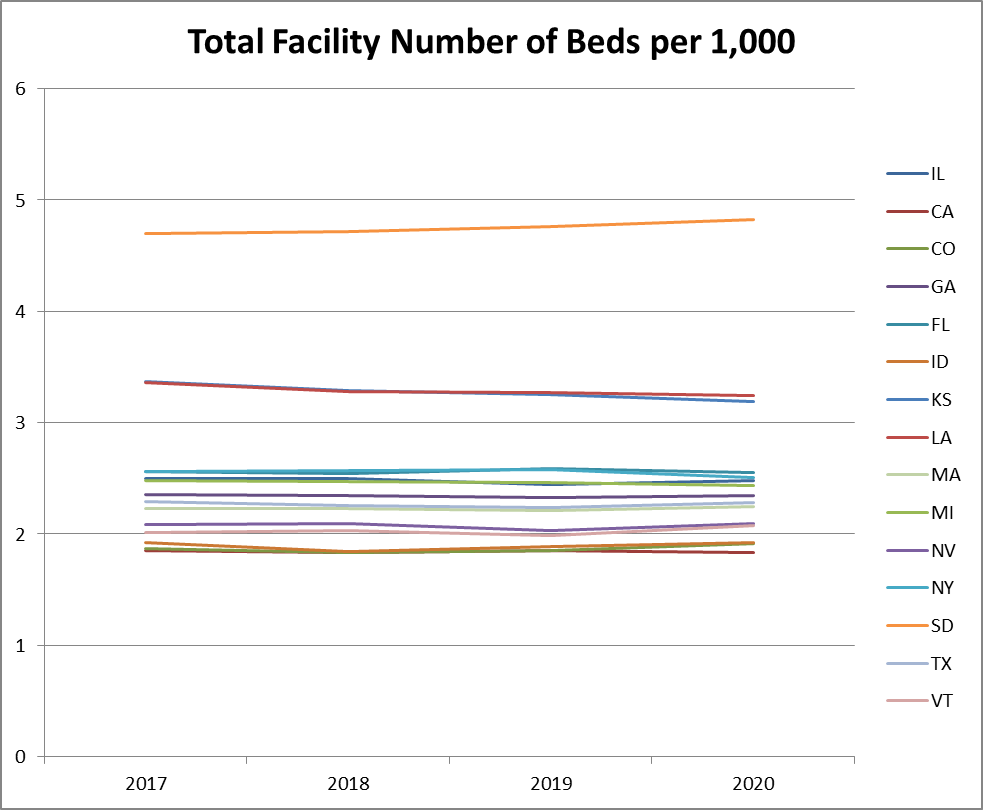
It’s plausible that hospitals would feel overrun if there were a significant decrease in hospital capacity. But in 2020, hospital capacity in most states was comparable to capacity in previous years.
A decrease in hospital personnel could also affect the ability of hospitals to operate efficiently. Perhaps during lockdowns, many nurses quit their positions to watch their children at home when schools were shut down.
However, employment levels at hospitals did not change much in 2020. Some states saw a decrease or an increase in personnel, but on average there was not much difference in 2020 compared to the three previous years.
Severity of Inpatient Stays
What is clear from the AHA data is that in most states, the average length of an inpatient stay in 2020 increased by about 5%. This implies that even though the number of hospital visits decreased in 2020, the average severity of each inpatient visit was higher than in previous years, which could contribute to doctors and nurses feeling overwhelmed. Most people would immediately attribute this increase in severity to COVID. In a future post, I am going to take a closer look at what exactly was going on in the hospitals during 2020, and whether there were other factors contributing to the massive amount of death taking place in the United States.
Regardless of the severity of inpatient cases, the total number of inpatient days still decreased in most states. This implies that hospitals were not overwhelmed compared to previous years.
Possible Explanations for the Panic
So why did we hear so many hospital horror stories, not just from the media, but from friends and family?
A few things to consider:
First, it’s important to remember that hospital workers have always had tough jobs. They have to work shifts that cover all hours of the day and many feel overworked. The prospect of having to work on the front lines during a pandemic was probably incredibly stressful and took a toll on these people.
Secondly, patients tended to stay longer at hospitals during 2020. This may have given the impression to hospital workers that more people were developing severe disease and dying than in previous years, which adds to the stress of the work environment.
Another point to consider is that while hospitals ought to take care of patients, they also need to make money. The healthcare system is bogged down by regulations and bureaucracy. Hospital managers are concerned with making their hospitals profitable. When government offers skewed incentives in response to a pandemic, it could translate into a more poorly run hospital, even though there are fewer patients than in previous years. In other words, the perception that hospitals were overwhelmed may have been due to bad management, not to an increase in the number of patients.
Finally, we can’t forget the impact that lockdowns had on society at large and how this relates back to healthcare. Hospitals are not islands. They require energy, supplies, and manpower. If there are disruptions in the supply chain, hospitals cannot acquire all the necessary supplies. If hospital employees are not able to participate in leisurely activities off the clock, it could affect their productivity at work. It may seem like the bowling alley, the café down the street, or the gardening store have nothing to do with hospitals, but in our interconnected world, they do have a tiny impact. Closing just one establishment won’t have much of an effect on overall healthcare. But when you close a whole host of businesses, the effect is compounded. Hospitals may still be able to operate, but if the economic environment on which they rely is severely maimed, it will affect how efficiently they are able to run
Notes:
The hospital utilization statistics are the “total facility” numbers and include nursing home units. The AHA also provides data for just hospital units, but it is not as comprehensive as the total facility data. I noticed that nursing home units were only a small fraction of the total facility utilization, so I decided to use the total facility numbers. If one were to plot the data from hospital units only, the same decrease in utilization in 2020 is apparent.
Anyone with a basic knowledge of numbers can look at the data from the AHA and realize that the hospitals in 2020 were not overflowing. Of course, the AHA consists of the very people who called for lockdowns, saying they were needed to keep the hospitals from being overrun. They try to save face with a disclaimer at the bottom of their page: The 2020 financial and performance data do not reflect the full impact of the COVID-19 pandemic. Right…