Panic and the Pathogen
The past three years saw a marked increase in death, but the debate about the exact cause of it all is still ongoing
A while back I mentioned that I would be looking more in depth as to why the length of inpatient hospital stays and excess deaths increased during the COVID period when COVID itself has a relatively low infection fatality ratio.
Many of us may have friends or family who worked in hospitals during 2020. For several of them, the low IFR is not easy to accept. If COVID was not very dangerous, then why did the hospitals seem to be overflowing with patients? Why were doctors and nurses working long, strenuous hours? Why were body bags stacking up in the hospitals? And why were there so many excess deaths, a trend that continues to this day?
Were all the severe illnesses and excess deaths over the past few years due to the virus? Or was there something else going on?
The Spring Wave
In early spring of 2020, as panic was spreading over COVID, many countries experienced a sudden and sharp peak in deaths. The curious thing about this wave of death was how uncharacteristic it was.
In the northern hemisphere, deaths typically rise in late autumn as colder weather arrives and peak during the winter, with a second smaller peak sometimes occurring in the spring. This seasonal wave of death is in large part due to respiratory illness and primarily affects the elderly.
As spring of 2020 approached, the seasonal wave of deaths was on the downward slope when suddenly, deaths spiked upward. The reason for this seemed very clear at the time: a novel, harmful respiratory virus was spreading, leading to severe illness and death.
However, there is quite a bit of evidence that by the time a pandemic was announced in March of 2020, COVID-19 had been spreading widely for several months.
For instance, Italian researchers discovered that in the supposed hotspot of Lombardy, Italy, COVID-19 had been circulating since September, 2019. By the time “Patient 1” tested positive in February 2020, researchers found evidence of “sustained transmission across all the Lombardy provinces.”
In addition, there is a anecdotal evidence from several people who claimed to get sick in early winter of 2019/2020 with a mysterious respiratory illness.
A.J. Kay documented how during that winter, hospital visits in the U.S. due to influenza-like illnesses increased in comparison to previous years, but positive tests for influenza did not increase with the same proportionality. This seemed to indicate that another respiratory illness was spreading during the winter of 2019, and this illness was most likely COVID-19.
It is possible that environmental conditions in late 2019 were not yet optimal for COVID to spread at an exponential rate, and that those conditions became optimal during the spring. That is at least what the Italian researchers concluded. COVID had apparently been sneaking around unnoticed for months when it suddenly decided to drop the hammer in March 2020.
I have a hard time believing this was the case. If COVID was already spreading widely by fall of 2019, why wouldn’t it peak in the middle of winter, just like many other respiratory viruses? Indeed, after COVID testing became widespread, even COVID itself peaked the following year in the winter of 2020/2021, and not in the spring. Why wasn’t the same thing happening the year before?
Additionally, why was COVID devastating certain hotspot areas like New York City, but not other populations located only a few hours away by car, such as New Hampshire or Vermont? If the virus spread for months, wouldn’t we have expected most of the neighboring populations to also have experienced a significant increase in deaths during this period?
And why are some countries such as the United Kingdom still experiencing significant excess mortality, even though COVID deaths have dropped?
The fact that COVID had been spreading for months before the spike in deaths raises the question of whether all those deaths could truly be attributed to the virus.
What the spike in deaths does correlate very closely with is the rising panic surrounding the virus. There is quite a bit of evidence showing that this panic had more to do with the climbing death toll than the virus itself.
In a world where we like to identify singular causes, it’s difficult to pinpoint how exactly a panic leads to excess death. That’s because a panic triggers not just one response, but a thousand responses, some of which could be harmful, while others are not.
As I have sifted through the various panic-induced responses during the COVID period, I’ve found the most harmful can be broken down into one or more of the following categories:
Mismanagement of hospitals
Harmful treatments
Isolation and movement restrictions
Failure to use standard treatments for respiratory illness
Hospital Mismanagement
Erin Olszewski was a nurse at the Elmhurst Hospital in New York City during the height of the pandemic. Elmhurst was considered the epicenter of the epicenter, and Olszewski took video recordings to document her experience.
What she uncovered was shocking.
Like many other hospitals, Elmhurst converted most of its wards to focus on COVID. Many inpatients tested negative for the virus upon arrival, but were recorded in the system as testing positive and moved to the COVID wing, where they eventually did get sick. Olszewski estimated that approximately half of the patients came to the hospital exhibiting symptoms of an anxiety attack, and many of them eventually underwent unnecessary treatment for COVID.
At Elmhurst and other US hospitals, the reason for inflating the COVID case numbers was clear. Hospitals received more government money for treating COVID patients, and they received even more if they treated a COVID patient with a ventilator. This incentivized hospitals to to be managed in a way that would actually lead to more respiratory illness, not less. Even though medical personnel may have been actively trying to save people’s lives, they were working in a system over which they had little influence, and which was designed to produce more COVID patients, not less. Hospital practices that may have inadvertently led to more disease and death would not be discontinued because the financial incentives did not encourage hospitals to make such corrections.
Olszewski also related that at her hospital, inexperienced doctors were playing a large role in the ICU. Residents would practice their newly acquired skills on the patients without the oversight of a more experienced doctor. This resulted in patients receiving low quality care, or in some cases receiving treatment that was unnecessary and potentially harmful.
Low quality care was enabled due to one of the worst panic-induced policies during this time: restricting hospital visits. Regardless of the severity of the government-imposed mandates, hospitals in several countries limited visits from family members and friends. Although the purpose of this policy was to limit the potential spread of the virus, it had a disastrous unintended consequence. Family members who visit loved ones in the hospital often are a source of oversight over doctors and nurses. Medical workers are human and make mistakes, and hospital visitors can put pressure on these workers to ensure that their loved ones receive proper medical care. During the COVID panic, since visitors were not allowed, this important layer of oversight was absent.
Harmful Treatements
At the beginning of the panic, many hospitals in hotspot areas were using ventilators on COVID patients. New York City and Lombardy in particular seemed to be using ventilators at a high rate. Although we don’t have an exact record of ventilator usage in these areas, media reports seemed to indicate that they were used more frequently than other locations. While ventilators seemed necessary in early 2020, it later became clear that they were hurting more than helping. It’s also possible that many hospitals were, like Elmhurst, unnecessarily putting ventilators on patients suffering from anxiety rather than from a respiratory illness. This only would have exacerbated the unnecessary harm done by ventilators in 2020.
In the United States, expensive and risky treatments were prioritized over repurposed drugs. Perhaps the most notorious was Remdesivir, an expensive antiviral developed during the 2014 Ebola outbreak that was associated with high death rates during testing. In November 2020, the WHO recommended against the use of Remdesivir in COVID-19 patients, and multiple studies have shown that it lead to life-threatening side effects. However, the drug was promoted heavily by Anthony Fauci, and American hospitals who treated with it would receive a 20% upcharge on the entire hospital bill, thus leading to its widespread usage in the U.S. Unfortunately, there is mounting evidence that widespread Remdesivir usage has led to increased renal failure and excess death in the United States.
Improper usage of Midazolam in treating patients has caused great concern in the United Kingdom. The National Institute for Health and Care Excellence (NICE) guideline NG163 was criticized by several doctors for its recommendation of pharmaceutical interventions intended for patients in the late stages of life. There are several allegations that utilizing these end-of-life care protocols amounted to euthanasia and have killed thousands of people.
Movement Restrictions and Immunity Debt
In the modern world, billions of people interact, trade, and travel all over the world. One consequence of this interconnectedness is that everyone is constantly exposed to a wide variety of pathogens. Our immune systems learn to defend against new, constantly evolving threats, and as a result, they become more robust.
The lockdowns and travel restrictions imposed by several countries all over the world discouraged movement between countries and interactions with a wide variety of people. This led to decreased exposure, and as a result, people’s immune systems became more naïve. Years of movement restrictions led to widespread immunity debt of the population, which subsequently led to more severe illness.
This is another factor contributing to excess death, even after COVID subsided. In 2022, when many countries no longer deemed COVID to be a threat and abandoned their restrictions, it seemed that sickness was more widespread than in previous years. For me personally, I got sicker in 2022 than I had in the past several years, and many others in my circle experienced the same thing.
As Jeffrey Tucker has often stated, the biggest health threat to humanity is not a killer virus, but a weak immune system. Years of lockdowns and movement restrictions prevented people from interacting, which led to a population with naïve immune systems, which resulted in more severe illness and death. This is I think one of the main reasons we saw significant excess deaths over the course of several years, when we should have seen a pull-over effect after that first initial wave.
Self-Isolation
While hospital mismanagement and risky treatments contributed to additional deaths during the COVID period, there is another response that I believe was even more consequential and dangerous. That was the widespread call for people with symptoms or who tested positive to self-isolate for two weeks.
All over the world, the average person was regularly told to self-isolate for two weeks if they tested positive for COVID. This was the common knowledge of the time, and for me, an average person, this was the main “treatment” I was ever aware of during all of 2020. The advice was very confusing and only led to more questions. Should I wait until it get’s really bad before seeing a doctor? Should I go outside and get some sunshine? Should I not make contact with anyone, even in my own household, for two weeks?
Why was self-isolation so dangerous? Because it discouraged people, particularly the elderly, from taking common sense approaches to treating their disease, such as getting help from a loved one, or seeing a doctor and getting medication if things were worsening after a few days. Sadly, because of the novel “common sense” advice to self-isolate for two weeks, many people waited at home alone, afraid, and sick until they couldn’t breathe, but by that point it was too late.
Failure to Use Standard Treatments
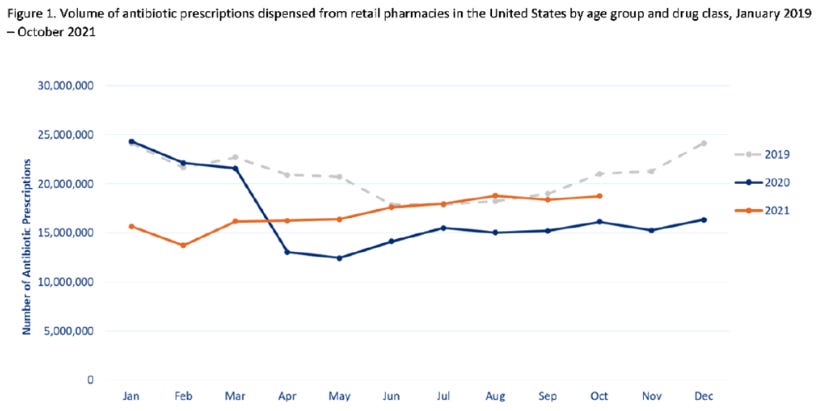
Evidence of the harmful effects of self-isolation can be found in the prescription data for antibiotics.
As I’ve written previously, antibiotic prescriptions decreased significantly in 2020 and 2021.
The Great Pneumonia Epidemic
COVID-19 has gotten an enormous amount of coverage over the past few years. Over 6 million deaths have been attributed to the disease, though it is unclear what percentage of those deaths could be solely attributed to COVID. During the panic, while everyone cowered in fear of the new disease, another common disease was killing more people than it had in …
This wasn’t necessarily because hospitals were abandoning standard remedies for respiratory illnesses in their effort to treat COVID. The CDC reported that approximately 80% of hospitalized COVID patients were receiving antibiotics. What changed drastically was the number of outpatient prescriptions.
The sharp decline in outpatient antibiotic prescriptions is likely due to the self-isolation guidance. Many people who fell ill were advised to stay home and stay isolated. As their respiratory illness developed into pneumonia, they did not receive standard treatments such as antibiotics until it was too late. For the elderly, this would have been particularly devastating, as they are the most at risk of dying from bacterial pneumonia.
Since the elderly are most at risk of contracting pneumonia, the drop in antibiotic prescriptions has led me to believe that COVID isn’t as deadly for the elderly as is commonly thought. If COVID was twice as deadly as the flu for those under 70, it seems reasonable to assume that this would also be the case for the elderly. Yes, I have heard some of the possible explanations for why COVID is particularly bad for the elderly, and perhaps they are true. But I think more likely, the COVID deaths for those over 70 were inflated due to them not receiving standard treatment for respiratory illness.
For many readers, what I’ve written here is nothing new. But most people, and even many skeptics, are still under the assumption that COVID was a unique killer somehow worthy of the panic. In reality, it was about twice as dangerous as the average flu. I don’t want to downplay the severity of the disease. Many people got sick, and many people died from it, just as many people die each year from respiratory illnesses.
But the real threat to humanity was not the virus itself.
The real threat was the response: the great panic, the power grabs by governments, and the military grade propaganda that bombarded the airwaves. The panic is what led health care providers to make harmful changes to their treatment protocols, and it discouraged people from taking common sense steps to seek proper treatment. Sadly, the panic is what exacerbated the death toll, making an albeit bad respiratory virus look far worse than it actually was.


Interestingly, Biobot Analytics, the company that performed early wastewater measurements of SARS-coV-2 concentration, has removed data from early 2020. As recently as March of this year, their data file showed no virus from 2020-01-15 to 2020-02-26 in the Boston area, but those dates have been removed.
https://raw.githubusercontent.com/biobotanalytics/covid19-wastewater-data/master/wastewater_by_county.csv
https://github.com/biobotanalytics/covid19-wastewater-data
Edit: The removal actually occured on 5/8/2023 in git commit 1ce4e2d. I had taken the zero measurements in early 2020 at face value and thought they were evidence against early spread. But apparently the story is more complicated. FWIW, here are the deleted lines:
sampling_week,effective_concentration_rolling_average,region,state,name,fipscode
2020-01-15,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-01-22,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-01-29,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-02-05,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-02-12,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-02-19,0.0,Northeast,MA,"Suffolk County, MA",25025
2020-02-26,0.0,Northeast,MA,"Suffolk County, MA",25025